Prinzmetal angina, also known as variant angina, is a rare type of chest pain caused by temporary narrowing or spasm of a coronary artery. Unlike other forms of angina, which are usually triggered by physical exertion or emotional stress, Prinzmetal angina occurs at rest or during sleep. The chest pain associated with Prinzmetal angina is often severe and sudden but typically lasts for only a few minutes. Understanding the causes of Prinzmetal angina is crucial in providing appropriate treatment and improving quality of life for individuals affected by it.
In this article, we will delve into the causes of Prinzmetal angina, how it affects the heart, and how it differs from other types of angina.
What Is Prinzmetal Angina?
Prinzmetal angina is a type of chest pain that occurs due to a spasm in a coronary artery, which temporarily restricts blood flow to the heart muscle. This spasm causes a reduction in oxygen delivery to the heart, leading to symptoms such as sharp chest pain or discomfort. It is important to note that Prinzmetal angina is a temporary condition, and the artery spasm usually resolves on its own.
Unlike stable angina, which occurs due to narrowed arteries from plaque buildup, Prinzmetal angina can happen even in people with healthy coronary arteries. This makes it a unique and less understood form of angina.
Causes of Prinzmetal Angina
Coronary Artery Spasm
The primary cause of Prinzmetal angina is the spasm of a coronary artery. In most cases, this occurs in the small branches of the arteries that supply blood to the heart. The spasm causes the artery to temporarily narrow, reducing blood flow to the heart. While the exact reason for these spasms is not fully understood, several factors are thought to contribute.
Abnormal Endothelial Function
The endothelium is the inner lining of blood vessels, including the coronary arteries. In healthy individuals, the endothelium produces substances that help regulate the size of blood vessels, allowing them to constrict and dilate as needed. In some people with Prinzmetal angina, however, the endothelium does not function properly, which can trigger abnormal vasoconstriction (narrowing of blood vessels).
This dysfunction may be influenced by genetic factors, lifestyle choices, or environmental conditions.
Increased Sympathetic Nervous System Activity
The sympathetic nervous system is responsible for the body’s “fight or flight” response, including raising the heart rate and increasing blood pressure. Overactivity of the sympathetic nervous system may cause the coronary arteries to constrict.
This may contribute to the development of Prinzmetal angina, as excessive nervous system stimulation can trigger spasm in the arteries.
Substance Abuse
Certain substances, particularly tobacco, cocaine, and other drugs that cause vasoconstriction, are strongly associated with Prinzmetal angina. These substances can provoke coronary artery spasms by stimulating the sympathetic nervous system or directly affecting the blood vessels. Cocaine, for example, is known to increase the likelihood of spasm in the coronary arteries and can trigger an episode of angina.
Cold Exposure
Exposure to cold temperatures can trigger a spasm in the coronary arteries in some people. This is because cold temperatures can cause the blood vessels to constrict in order to conserve heat. In susceptible individuals, this constriction can extend to the coronary arteries, reducing blood flow to the heart and causing chest pain.
Hyperventilation and Stress
Breathing in excessively fast or shallow, especially in stressful situations, can cause the coronary arteries to constrict.
Additionally, stress can lead to the release of stress hormones such as adrenaline, which can also contribute to spasm of the arteries. While stress and hyperventilation are not as common as other triggers, they can still play a role in precipitating Prinzmetal angina.
Other Underlying Health Conditions
Certain health conditions may increase the likelihood of developing Prinzmetal angina. These include:
Atherosclerosis: While atherosclerosis (plaque buildup) is not the primary cause of Prinzmetal angina, individuals with existing plaque buildup may be at higher risk for coronary artery spasm.
Atherosclerosis can damage the endothelial lining of the arteries, making them more prone to spasm.
Migraines: There is a known association between Prinzmetal angina and migraines. It is believed that the same factors that contribute to migraines, such as abnormal vascular responses, may also play a role in triggering coronary artery spasm.
Raynaud’s Disease: This condition, which affects blood flow to the extremities, can also be linked to Prinzmetal angina.
Individuals with Raynaud’s disease experience episodes of narrowed blood vessels, which can sometimes affect the coronary arteries as well.
Diabetes: Diabetes, particularly when poorly controlled, can lead to vascular dysfunction, including abnormal endothelial function. This dysfunction may contribute to the development of Prinzmetal angina in individuals with the condition.
Symptoms of Prinzmetal Angina
The hallmark symptom of Prinzmetal angina is sudden chest pain, which usually occurs at rest or during sleep. The pain can last anywhere from a few minutes to about 15 minutes and often subsides on its own. While the chest pain can be intense, it is typically not associated with physical exertion.
The pain may be accompanied by other symptoms such as shortness of breath, dizziness, or lightheadedness. However, many individuals with Prinzmetal angina experience no long-term damage to the heart, as the coronary artery spasm is temporary and often resolves quickly.
Diagnosis of Prinzmetal Angina
Diagnosing Prinzmetal angina typically involves a combination of medical history, physical examination, and tests to evaluate the heart’s function. These tests may include:
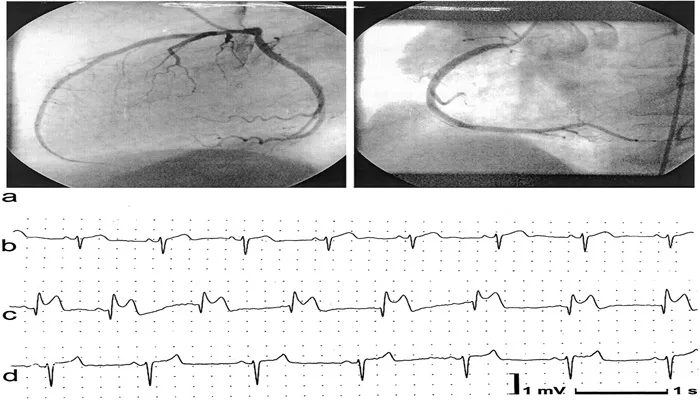
Electrocardiogram (ECG): An ECG is used to measure the electrical activity of the heart. During a spasm, changes may appear on the ECG, helping doctors diagnose Prinzmetal angina.
Coronary Angiography: In some cases, a coronary angiogram may be performed to visualize the coronary arteries and identify any signs of spasm or narrowing.
Stress Testing: While stress tests are generally used to evaluate stable angina, they may also help identify abnormal blood flow patterns that suggest Prinzmetal angina. However, stress testing may not always trigger a spasm, as these episodes often occur at rest.
Treatment of Prinzmetal Angina
The main goal of treatment for Prinzmetal angina is to reduce or eliminate the frequency of coronary artery spasms. This can be achieved through the use of medications that help relax the blood vessels and prevent spasms. These treatments may include:
Calcium Channel Blockers: These medications help relax the smooth muscles in the blood vessels, reducing the likelihood of spasm.
Nitrates: Nitrates are commonly used to dilate the coronary arteries and relieve chest pain associated with angina.
Statins: In some cases, statins may be prescribed to reduce cholesterol levels and prevent the development of atherosclerosis, which could exacerbate Prinzmetal angina.
Lifestyle Changes: While lifestyle changes may not directly prevent coronary artery spasm, they can help manage other risk factors for heart disease, such as smoking, high cholesterol, and hypertension.
Conclusion
Prinzmetal angina is a rare but serious condition that is caused by temporary coronary artery spasm. Various factors, including abnormal endothelial function, increased sympathetic nervous system activity, and substance abuse, can trigger these spasms. Although the condition can be alarming due to the intensity of the chest pain, it is typically treatable with medications and lifestyle modifications. Early diagnosis and appropriate treatment can help manage the symptoms and reduce the frequency of episodes, allowing individuals with Prinzmetal angina to lead healthier lives.
Related topics: