Paroxysmal atrial tachycardia (PAT) is a condition in which the heart experiences sudden, rapid heartbeats originating from the atria, the upper chambers of the heart. This rapid heart rate, often over 100 beats per minute, can be alarming to those experiencing it, as it can come on suddenly and last for a few seconds to several minutes. While many factors can trigger PAT, one of the less commonly discussed but highly relevant causes is stress. This article aims to explore the connection between stress and paroxysmal atrial tachycardia, outlining the mechanisms behind this association, symptoms, diagnosis, and potential treatment options.
Understanding Paroxysmal Atrial Tachycardia
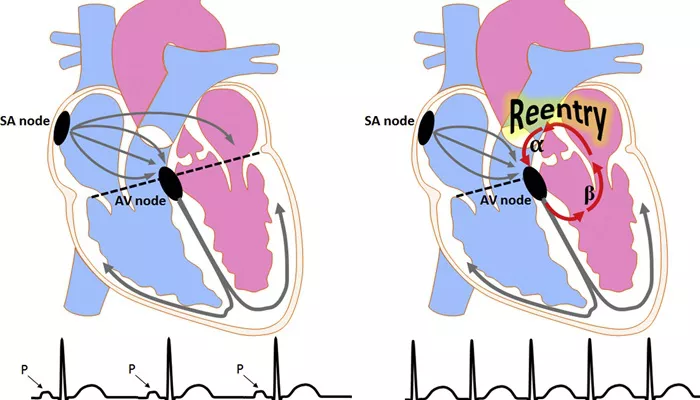
Before delving into the role of stress, it’s essential to understand what paroxysmal atrial tachycardia is and how it affects the heart. PAT is a form of arrhythmia, or an irregular heartbeat, characterized by rapid electrical impulses originating in the atria. These impulses override the heart’s normal rhythm and cause the heart rate to accelerate unexpectedly.
PAT can occur in people who are otherwise healthy, though it may be more prevalent in individuals with underlying heart conditions or other arrhythmias. It typically starts suddenly and ends abruptly, often without any clear warning signs. The episode can last from a few seconds to several minutes, and in some cases, it can even last longer.
There are three main types of PAT:
Focal Atrial Tachycardia: Caused by a single, abnormal focus in the atria.
Multifocal Atrial Tachycardia (MAT): Caused by multiple abnormal foci in the atria.
Atrioventricular Nodal Reentrant Tachycardia (AVNRT): A type of reentrant arrhythmia involving the atrioventricular node.
How Does Stress Affect the Heart?
Stress, especially chronic or acute stress, has a significant impact on the cardiovascular system. It triggers a series of physiological responses in the body, many of which can potentially lead to arrhythmias such as PAT. The primary mechanism through which stress affects the heart is through the release of stress hormones, particularly adrenaline (also known as epinephrine) and cortisol.
When you experience stress, whether physical or emotional, the body enters a “fight or flight” mode. This response is designed to prepare the body to respond to perceived threats. Adrenaline is released from the adrenal glands, which accelerates the heart rate, increases blood pressure, and heightens alertness. While these responses are helpful in short bursts, they can become harmful if prolonged or chronic.
Stress also affects the autonomic nervous system (ANS), which controls involuntary functions such as heart rate and digestion. The ANS consists of two branches: the sympathetic nervous system (SNS) and the parasympathetic nervous system (PNS). The SNS is responsible for the body’s stress response, increasing heart rate and preparing the body for action, while the PNS works to calm the body down and reduce heart rate.
In situations of stress, the SNS tends to dominate, leading to a heightened state of arousal that can disrupt the normal rhythm of the heart. This imbalance in autonomic control can contribute to the development of arrhythmias like PAT.
The Link Between Stress and Paroxysmal Atrial Tachycardia
Several studies and clinical observations suggest that stress can trigger paroxysmal atrial tachycardia. The underlying mechanism often involves a heightened sympathetic response, which can create an environment conducive to arrhythmias.
Here are some ways stress can contribute to PAT:
Increased Heart Rate and Blood Pressure: The immediate response to stress is an increase in heart rate and blood pressure, which can trigger abnormal electrical activity in the atria, leading to a tachycardic episode.
Autonomic Nervous System Imbalance: As mentioned earlier, stress activates the sympathetic nervous system, which can overpower the parasympathetic system, causing a disruption in the normal electrical conduction in the heart. This disruption can lead to the development of PAT.
Electrophysiological Changes in the Heart: Chronic stress may lead to long-term changes in the electrophysiological properties of the heart.
This includes alterations in ion channel function and increased sensitivity to abnormal electrical signals, making the heart more susceptible to arrhythmias.
Inflammation and Hormonal Changes: Chronic stress is known to cause low-grade inflammation in the body, which may affect the heart’s electrical pathways. Additionally, elevated cortisol levels, which are common in times of stress, can also contribute to arrhythmias by altering the heart’s rhythm and electrical conduction.
Symptoms of Paroxysmal Atrial Tachycardia
When an episode of PAT occurs, it often presents with the following symptoms:
Sudden Rapid Heartbeat: A noticeable increase in heart rate, often exceeding 100 beats per minute, which may feel like a racing or pounding heart.
Dizziness or Lightheadedness: The rapid heart rate may reduce the efficiency of the heart’s pumping action, leading to decreased blood flow and symptoms like dizziness.
Shortness of Breath: As the heart struggles to pump effectively, individuals may experience difficulty breathing or a sensation of breathlessness.
Chest Discomfort or Pain: Some individuals may feel tightness or discomfort in the chest, although chest pain is more commonly associated with other heart conditions.
Fatigue or Weakness: Due to the heart’s reduced efficiency, a person may feel unusually tired or weak during or after an episode of PAT.
Stress-Induced Paroxysmal Atrial Tachycardia: Risk Factors
While stress can cause PAT, certain risk factors may make individuals more susceptible to experiencing episodes. These risk factors include:
Pre-existing Heart Conditions: People with underlying heart disease or a history of arrhythmias are more likely to develop PAT when exposed to stress.
High Levels of Chronic Stress: Individuals who regularly experience high levels of emotional or physical stress are at an increased risk of developing PAT.
Family History of Arrhythmias: A genetic predisposition to arrhythmias can make individuals more vulnerable to PAT when under stress.
Caffeine, Alcohol, and Drug Use: Stimulants such as caffeine or alcohol, as well as certain recreational drugs, can exacerbate the effects of stress on the heart, increasing the likelihood of a PAT episode.
Diagnosis of Paroxysmal Atrial Tachycardia
If you suspect that stress is causing paroxysmal atrial tachycardia, it is important to consult with a healthcare provider for a proper diagnosis.
Several diagnostic tools can be used to confirm PAT:
Electrocardiogram (ECG): The primary diagnostic tool for arrhythmias, including PAT, is an ECG. This test records the electrical activity of the heart and can reveal any abnormal heart rhythms during an episode.
Holter Monitor: A portable device worn for 24 to 48 hours that continuously records the heart’s electrical activity. This test is useful in detecting intermittent arrhythmias that may not be captured during a standard ECG.
Echocardiogram: This imaging test uses sound waves to create a picture of the heart, which can help rule out any underlying structural issues contributing to PAT.
Stress Test: A test that monitors heart function while the body is subjected to physical exertion or stress. It can help identify if stress or exercise triggers arrhythmias.
Treatment Options for Stress-Induced Paroxysmal Atrial Tachycardia
The treatment for paroxysmal atrial tachycardia triggered by stress involves both addressing the underlying arrhythmia and managing the stress itself. Possible treatment options include:
Vagal Maneuvers: These are techniques that help to stimulate the parasympathetic nervous system and restore normal heart rhythm. Examples include coughing, bearing down as if having a bowel movement, or applying cold water to the face.
Medications: Antiarrhythmic drugs may be prescribed to control the frequency and duration of PAT episodes. Beta-blockers and calcium channel blockers can help regulate the heart rate, while other medications may be used to manage stress or anxiety.
Catheter Ablation: In some cases, if the PAT episodes are frequent or severe, a procedure called catheter ablation may be recommended. This involves using a catheter to destroy the abnormal tissue in the heart responsible for triggering the arrhythmia.
Stress Management Techniques: Since stress is a primary trigger for PAT in some individuals, incorporating relaxation techniques such as yoga, meditation, and deep breathing exercises can be beneficial in reducing the frequency and intensity of episodes.
Conclusion
Stress is indeed a significant factor in triggering paroxysmal atrial tachycardia in susceptible individuals. The mechanisms through which stress influences the heart are complex but involve the activation of the sympathetic nervous system and the release of stress hormones like adrenaline. While PAT is a treatable condition, it is essential for those experiencing it to seek medical advice for proper diagnosis and management. Reducing stress through lifestyle changes, relaxation techniques, and medical interventions can help mitigate the risk of PAT episodes and improve overall cardiovascular health.
Related topics: