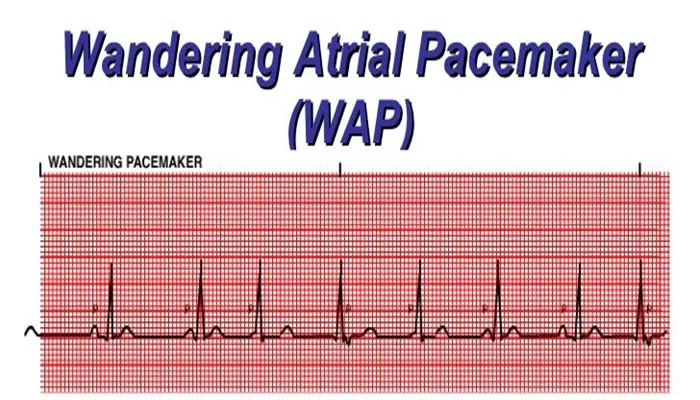
In the realm of cardiology, understanding the various types of cardiac rhythms and their underlying mechanisms is crucial for diagnosing and managing heart conditions. One interesting and somewhat complex phenomenon is the wandering atrial pacemaker (WAP). This article will explore the definition, causes, clinical significance, diagnosis, treatment options, and management strategies related to wandering atrial pacemaker. By the end, readers will have a comprehensive understanding of this unique cardiac rhythm and its implications for patient care.
Understanding Cardiac Pacemakers
What Are Cardiac Pacemakers
Cardiac pacemakers are specialized cells in the heart that generate electrical impulses, initiating the heart’s contraction and maintaining a regular heartbeat. The primary pacemaker of the heart is the sinoatrial (SA) node, located in the right atrium. However, other areas of the heart can also act as pacemakers under certain conditions, leading to various arrhythmias.
The Role of the Sinoatrial Node
The SA node is responsible for setting the normal rhythm of the heart, typically firing at a rate of 60 to 100 beats per minute. It sends electrical signals through the atria, causing them to contract and push blood into the ventricles. The electrical impulses then travel to the atrioventricular (AV) node, which acts as a gatekeeper, allowing impulses to pass into the ventricles at a controlled rate.
What Is Wandering Atrial Pacemaker
Definition of Wandering Atrial Pacemaker
Wandering atrial pacemaker (WAP) is a type of arrhythmia characterized by the shifting of the primary pacemaker site from the SA node to other areas within the atria. This phenomenon results in varying P-wave morphology on an electrocardiogram (ECG), as different pacemaker sites generate electrical impulses with slightly different characteristics.
Characteristics of Wandering Atrial Pacemaker
WAP is defined by the following characteristics:
Variable P-Wave Morphology: The P waves on the ECG show different shapes and sizes, reflecting the different origins of the electrical impulses.
Heart Rate: The heart rate in WAP is typically between 60 and 100 beats per minute, although it can be slower or faster depending on the underlying cause.
Irregular Rhythm: The rhythm may appear irregular due to the changing pacemaker sites, leading to variations in the timing of the P waves.
Types of Atrial Pacemakers
The wandering atrial pacemaker can be distinguished from other types of atrial pacemakers, including:
Sinoatrial Node Pacemaker: The primary pacemaker, firing at a consistent rate with uniform P waves.
Ectopic Atrial Pacemaker: An abnormal pacemaker site in the atria that can take over the pacing of the heart, typically resulting in a more consistent P wave morphology.
Causes of Wandering Atrial Pacemaker
Physiological Causes
Wandering atrial pacemaker can occur in healthy individuals, particularly during sleep or relaxation. It is often considered a benign condition and may not require treatment. Factors that can contribute to WAP include.
Respiratory Variations: Changes in intrathoracic pressure during breathing can influence the autonomic nervous system, leading to variations in heart rate and pacemaker activity.
Physiological Stress: Situations such as exercise, anxiety, or emotional stress can temporarily alter the site of pacemaker activity.
Pathological Causes
While WAP is often benign, it can also be associated with certain pathological conditions, including:
Atrial Enlargement: Conditions that cause atrial enlargement, such as mitral valve disease or heart failure, can lead to ectopic pacemaker activity.
Hypoxia: Low oxygen levels in the blood can stimulate ectopic pacemakers, resulting in WAP.
Electrolyte Imbalances: Abnormal levels of potassium, magnesium, or calcium can affect the heart’s electrical activity, contributing to WAP.
Medications: Certain medications, particularly those that affect the autonomic nervous system, can lead to changes in pacemaker activity.
Clinical Significance of Wandering Atrial Pacemaker
Diagnosis and Symptoms
Wandering atrial pacemaker is often asymptomatic, particularly in healthy individuals. However, symptoms may arise if the heart rate becomes significantly irregular or if the underlying cause is related to a more serious condition. Common symptoms may include:
- Palpitations
- Dizziness or lightheadedness
- Fatigue
- Shortness of breath
Diagnostic Evaluation
The diagnosis of wandering atrial pacemaker is primarily based on an electrocardiogram (ECG). Key diagnostic features include.
Variable P Waves: The presence of P waves with different morphologies, indicating the shifting pacemaker sites.
Irregular Rhythm: The overall rhythm may appear irregular, with varying intervals between QRS complexes.
Normal QRS Complexes: The QRS complexes are typically narrow and normal, indicating that the electrical impulses are conducted properly through the ventricles.
Differential Diagnosis
When evaluating a patient with suspected wandering atrial pacemaker, it is essential to differentiate it from other arrhythmias, such as.
Multifocal Atrial Tachycardia (MAT): Similar to WAP, but characterized by a heart rate greater than 100 beats per minute and more pronounced P-wave variability.
Atrial Flutter: A reentrant arrhythmia that produces a rapid and regular atrial rate, typically with a “sawtooth” pattern on the ECG.
Atrial Fibrillation: An irregularly irregular rhythm with no discernible P waves, often associated with a higher risk of stroke.
Treatment of Wandering Atrial Pacemaker
General Management
In most cases, wandering atrial pacemaker is a benign condition that does not require treatment. If the patient is asymptomatic and the WAP is not associated with any underlying pathology, no intervention is necessary. However, the following management strategies may be considered.
Monitoring: Regular follow-up and monitoring of the patient’s condition may be recommended, particularly if there are any changes in symptoms or clinical status.
Lifestyle Modifications: Encouraging patients to adopt a heart-healthy lifestyle, including regular exercise, a balanced diet, and stress management techniques, can help improve overall cardiovascular health.
Treatment of Underlying Causes
If wandering atrial pacemaker is associated with an underlying pathological condition, addressing that condition is essential. Treatment options may include.
Medications: If electrolyte imbalances or other medical conditions are contributing to WAP, appropriate medications may be prescribed to correct these issues.
Management of Heart Disease: Patients with underlying heart conditions, such as heart failure or valvular disease, may require specific treatments to improve their overall heart function.
Advanced Interventions
In rare cases where WAP is symptomatic or associated with significant cardiac dysfunction, more advanced interventions may be necessary.
Catheter Ablation: If ectopic atrial pacemaker activity is causing significant symptoms or complications, catheter ablation may be considered to eliminate the abnormal pacemaker site.
Pacemaker Implantation: In patients with persistent symptoms and underlying conduction system disease, permanent pacemaker implantation may be indicated to maintain an appropriate heart rate.
Long-Term Management and Follow-Up
Regular Follow-Up
Patients diagnosed with wandering atrial pacemaker should have regular follow-up appointments to monitor their heart health and assess any changes in symptoms. Follow-up care may include.
Electrocardiograms: Routine ECGs can help track any changes in heart rhythm and ensure that WAP remains stable.
Symptom Assessment: Patients should be encouraged to report any new or worsening symptoms, such as palpitations, dizziness, or shortness of breath.
Lifestyle Modifications
Encouraging patients to adopt a heart-healthy lifestyle can significantly impact their overall well-being and cardiovascular health. Key lifestyle modifications may include.
Diet: A balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can support heart health.
Exercise: Regular physical activity can improve cardiovascular fitness and help manage weight.
Stress Management: Techniques such as yoga, meditation, and deep breathing exercises can help reduce stress and promote relaxation.
Avoiding Stimulants: Limiting caffeine and other stimulants can help reduce the frequency of ectopic beats and improve overall heart rhythm.
Patient Education
Educating patients about their condition is essential for promoting adherence to follow-up care and encouraging lifestyle modifications. Key points for patient education may include.
Understanding the nature of wandering atrial pacemaker and its benign nature in most cases.
Recognizing the importance of regular follow-up and monitoring for any changes in symptoms.
Learning to identify potential triggers for arrhythmias and how to manage them.
Conclusion
Wandering atrial pacemaker is a unique cardiac phenomenon characterized by the shifting of the primary pacemaker site within the atria, leading to variable P-wave morphology and an irregular heart rhythm. While often benign and asymptomatic, WAP can be associated with underlying conditions that require attention.
Understanding the causes, clinical significance, diagnosis, and management of wandering atrial pacemaker is crucial for healthcare providers to ensure optimal patient care. In most cases, monitoring and lifestyle modifications are sufficient to manage this condition. However, addressing any underlying issues is essential for preventing complications and improving overall cardiovascular health.
As our understanding of cardiac rhythms continues to evolve, staying informed about conditions like wandering atrial pacemaker is vital for providing comprehensive care to patients with arrhythmias. By fostering a collaborative approach between patients and healthcare providers, we can enhance outcomes and promote a better quality of life for those affected by this intriguing cardiac phenomenon.
Related Topics: