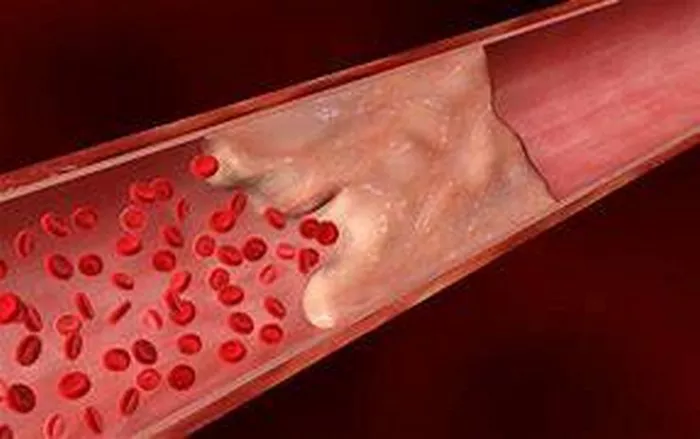
Calcification of the arteries, often referred to as vascular calcification, is a significant condition that poses serious risks to cardiovascular health. It involves the deposition of calcium salts in the arterial walls, leading to the hardening and stiffening of the arteries. This process can contribute to the development of atherosclerosis, increase the risk of cardiovascular events, and complicate the management of various medical conditions. Understanding the seriousness of arterial calcification, its causes, consequences, and management strategies is essential for promoting cardiovascular health and preventing severe complications.
What is Arterial Calcification
Definition
Arterial calcification is the accumulation of calcium phosphate crystals in the arterial walls. This pathological process can occur in various forms, including:
Intimal Calcification: This type occurs within the intima, the innermost layer of the artery, and is often associated with atherosclerosis. It typically develops in response to lipid accumulation and inflammation.
Medial Calcification: Also known as Monckeberg’s sclerosis, this type occurs in the medial layer of the arterial wall and is characterized by the deposition of calcium in the smooth muscle cells. Medial calcification is commonly seen in aging and conditions such as diabetes and chronic kidney disease.
Mechanisms of Calcification
The process of arterial calcification is complex and involves several mechanisms:
Cellular Changes: Vascular smooth muscle cells (VSMCs) can undergo phenotypic changes, transforming into osteoblast-like cells that promote calcification.
Inflammation: Chronic inflammation plays a crucial role in the calcification process. Inflammatory cytokines can stimulate VSMCs and promote the deposition of calcium.
Oxidative Stress: Increased oxidative stress can lead to endothelial dysfunction and contribute to vascular calcification.
Metabolic Factors: Conditions such as hyperphosphatemia (elevated phosphate levels), hypercalcemia (elevated calcium levels), and vitamin K deficiency can promote arterial calcification.
Causes of Arterial Calcification
Several factors contribute to the development of arterial calcification:
Age
As individuals age, the risk of arterial calcification increases. The accumulation of calcium in the arteries is a common finding in older adults, often leading to stiffened arteries and reduced elasticity.
Chronic Kidney Disease (CKD)
Patients with CKD are at a significantly higher risk of vascular calcification due to imbalances in calcium and phosphate metabolism. The kidneys play a crucial role in regulating these minerals, and their dysfunction can lead to hyperphosphatemia and subsequent calcification.
Diabetes Mellitus
Diabetes is associated with various metabolic changes that promote arterial calcification. High blood sugar levels can lead to glycation of proteins, inflammation, and oxidative stress, all of which contribute to vascular damage and calcification.
Atherosclerosis
Atherosclerosis, characterized by the buildup of fatty plaques in the arteries, is closely linked to arterial calcification. As plaques develop, they can become calcified, further narrowing the arteries and increasing the risk of cardiovascular events.
Hypertension
High blood pressure can lead to endothelial injury and promote the calcification process. The mechanical stress on arterial walls from hypertension can contribute to vascular remodeling and calcification.
Lifestyle Factors
Diet: Diets high in processed foods, sugars, and unhealthy fats can contribute to metabolic disorders that promote calcification.
Smoking: Tobacco use is associated with increased inflammation and oxidative stress, both of which can accelerate arterial calcification.
Sedentary Lifestyle: Lack of physical activity is linked to obesity, diabetes, and cardiovascular disease, all of which increase the risk of arterial calcification.
Consequences of Arterial Calcification
Arterial calcification can have several serious consequences for cardiovascular health:
Increased Risk of Cardiovascular Disease
Calcification is a significant predictor of cardiovascular events, including heart attacks and strokes. Studies have shown that individuals with higher levels of arterial calcification have an increased risk of developing coronary artery disease (CAD) and other cardiovascular conditions.
Reduced Arterial Elasticity
Calcified arteries lose their elasticity, making it more challenging for the heart to pump blood effectively. This reduced elasticity can lead to increased blood pressure and strain on the heart, contributing to heart failure.
Complicated Atherosclerosis
Calcification can complicate the atherosclerotic process. When plaques become calcified, they may become more stable and less likely to rupture; however, the presence of calcification can also indicate advanced atherosclerosis. This duality makes management more complex.
Impaired Blood Flow
Severe calcification can lead to significant narrowing of the arteries, restricting blood flow to vital organs and tissues. This can result in symptoms such as angina (chest pain) and claudication (pain in the legs during physical activity).
Increased Surgical Risks
Patients with significant arterial calcification may face increased risks during surgical procedures, such as angioplasty or bypass surgery. Calcified arteries can be more challenging to navigate and manage during interventions.
Diagnosis of Arterial Calcification
Imaging Techniques
Several imaging modalities are used to assess arterial calcification:
X-ray: While not the most sensitive method, X-rays can reveal calcifications in larger arteries.
Ultrasound: Vascular ultrasound can assess the presence of calcification in peripheral arteries.
CT Scan: Computed tomography (CT) scans, particularly coronary artery calcium (CAC) scoring, are widely used to quantify calcification in coronary arteries. A higher CAC score correlates with an increased risk of cardiovascular events.
MRI: Magnetic resonance imaging (MRI) can provide detailed images of arterial structures and detect calcification.
Blood Tests
Blood tests may be performed to evaluate calcium and phosphate levels, as well as other markers of cardiovascular risk, such as lipid profiles and inflammatory markers.
Management of Arterial Calcification
Lifestyle Modifications
Dietary Changes: A heart-healthy diet rich in fruits, vegetables, whole grains, and healthy fats can help manage risk factors associated with arterial calcification. Reducing intake of processed foods, sugars, and unhealthy fats is essential.
Regular Exercise: Engaging in regular physical activity can improve cardiovascular health and help manage conditions such as obesity, diabetes, and hypertension.
Smoking Cessation: Quitting smoking is one of the most effective ways to reduce cardiovascular risk and improve overall health.
Medical Management
Medications: Depending on the underlying conditions contributing to arterial calcification, medications may be prescribed to manage cholesterol levels, blood pressure, and diabetes.
Phosphate Binders: For patients with chronic kidney disease, phosphate binders may be used to help control phosphate levels and reduce the risk of calcification.
Vitamin K: Some studies suggest that vitamin K may play a role in inhibiting vascular calcification. However, more research is needed to establish its efficacy and appropriate dosing.
Regular Monitoring
Patients at risk for arterial calcification should undergo regular monitoring to assess cardiovascular health and identify any changes in arterial calcification. This may include routine imaging studies and blood tests.
Interventional Procedures
In cases of significant arterial blockage due to calcification, interventional procedures such as angioplasty or bypass surgery may be necessary. These procedures aim to restore blood flow and alleviate symptoms.
Conclusion
Calcification of the arteries is a serious condition that poses significant risks to cardiovascular health. It is a complex process influenced by various factors, including age, chronic diseases, lifestyle choices, and underlying atherosclerosis. The consequences of arterial calcification can be severe, leading to increased cardiovascular events, reduced arterial elasticity, and impaired blood flow.
Understanding the seriousness of arterial calcification emphasizes the importance of preventive measures and lifestyle modifications. Individuals can significantly reduce their risk of arterial calcification and its associated complications by adopting heart-healthy habits, managing chronic conditions, and undergoing regular health screenings.
Healthcare professionals play a crucial role in identifying at-risk individuals, providing appropriate interventions, and promoting awareness of the importance of maintaining vascular health. Through a combination of lifestyle changes, medical management, and regular monitoring, it is possible to mitigate the risks associated with arterial calcification and promote long-term cardiovascular health.
Related Topics: