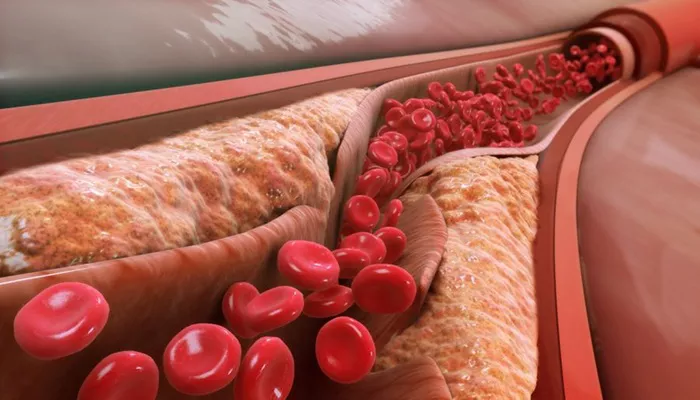
Atherosclerosis is a chronic condition characterized by the buildup of plaques within the arterial walls, leading to narrowed and hardened arteries. This process significantly increases the risk of cardiovascular diseases, including heart attacks and strokes. Given the serious implications of atherosclerosis, many individuals wonder: will atherosclerosis ever go away? This article explores the nature of atherosclerosis, its progression, treatment options, and the potential for reversal or management of the condition.
Understanding Atherosclerosis
Definition
Atherosclerosis is a progressive disease that begins with damage to the endothelium, the inner lining of the arteries. This damage can be caused by various risk factors, including high blood pressure, high cholesterol, smoking, diabetes, and inflammation. Over time, fatty deposits, cholesterol, calcium, and cellular debris accumulate at the site of injury, forming plaques that can obstruct blood flow.
Pathophysiology of Atherosclerosis
Endothelial Injury: The process of atherosclerosis begins with injury to the endothelial cells. Factors such as oxidative stress, high levels of low-density lipoprotein (LDL) cholesterol, and hypertension contribute to this damage.
Lipid Accumulation: Once the endothelium is damaged, LDL cholesterol infiltrates the arterial wall. Oxidized LDL triggers an inflammatory response, attracting immune cells to the site.
Inflammatory Response: Monocytes migrate to the site of injury and differentiate into macrophages, which engulf oxidized LDL, transforming into foam cells. The accumulation of foam cells forms fatty streaks in the arteries.
Plaque Formation: As foam cells die and release their contents, a necrotic core forms within the plaque. Smooth muscle cells migrate to the site and proliferate, forming a fibrous cap over the plaque.
Plaque Growth and Complications: Plaques can grow over time, leading to further narrowing of the arteries. They can also become unstable and rupture, causing thrombosis (blood clot formation) that can obstruct blood flow.
The Progression of Atherosclerosis
Stages of Atherosclerosis
Atherosclerosis progresses through several stages, and understanding these stages can provide insight into whether the condition can be reversed or managed.
Early Stage: In the initial phase, fatty streaks may form in the arteries, often without noticeable symptoms. This stage can begin in childhood and is influenced by genetic and lifestyle factors.
Intermediate Stage: As plaques develop, they can begin to obstruct blood flow. Individuals may start to experience symptoms such as angina (chest pain) or intermittent claudication (leg pain during exercise).
Advanced Stage: In the advanced stage, plaques can become large and unstable, increasing the risk of rupture. This can lead to acute cardiovascular events, such as heart attacks or strokes.
Complicated Atherosclerosis: At this stage, the plaques may cause significant obstruction of blood flow and complications such as thrombosis, aneurysms, or critical limb ischemia.
Factors Influencing Progression
The progression of atherosclerosis is influenced by a combination of genetic, environmental, and lifestyle factors. Key risk factors include:
Genetics: Family history of cardiovascular disease can increase an individual’s risk of developing atherosclerosis.
Diet: A diet high in saturated fats, trans fats, and cholesterol can contribute to elevated LDL levels and promote plaque formation.
Physical Inactivity: Sedentary lifestyles are associated with obesity, hypertension, and dyslipidemia, all of which increase the risk of atherosclerosis.
Smoking: Tobacco use is a significant risk factor for endothelial injury and promotes inflammation.
Chronic Conditions: Conditions such as diabetes, hypertension, and hyperlipidemia contribute to the development and progression of atherosclerosis.
Can Atherosclerosis Be Reversed
The Concept of Reversal
The term “reversal” in the context of atherosclerosis refers to the reduction or stabilization of plaque burden and improvement in arterial health. While complete reversal of atherosclerosis may not be achievable for everyone, significant improvements in cardiovascular health can be made through lifestyle changes and medical interventions.
Evidence of Plaque Regression
Research has shown that it is possible for atherosclerotic plaques to regress under certain conditions. Some key studies and findings include.
Lifestyle Interventions: Studies have demonstrated that intensive lifestyle changes, including dietary modifications, increased physical activity, and smoking cessation, can lead to regression of coronary artery disease. The Lifestyle Heart Trial, for example, showed that participants who adopted a plant-based diet experienced significant improvements in coronary artery health.
Pharmacological Interventions: Statins and other lipid-lowering medications have been shown to stabilize plaques and reduce cardiovascular events. Some studies suggest that aggressive lipid-lowering therapy can lead to plaque regression.
Advanced Imaging Techniques: Imaging studies using intravascular ultrasound (IVUS) and magnetic resonance imaging (MRI) have shown that changes in plaque volume can occur with appropriate interventions. These techniques allow for the assessment of plaque characteristics and changes over time.
Factors Influencing Reversal
The potential for plaque regression is influenced by several factors:
Duration of Disease: Individuals with early-stage atherosclerosis may have a better chance of regression compared to those with advanced disease.
Adherence to Treatment: Consistent adherence to lifestyle changes and medical therapies is crucial for achieving improvements in cardiovascular health.
Genetic Predisposition: Genetic factors may influence an individual’s response to interventions and their overall risk of cardiovascular disease.
Comorbid Conditions: The presence of other chronic conditions, such as diabetes or chronic kidney disease, can complicate the management of atherosclerosis and affect the potential for regression.
Management Strategies for Atherosclerosis
Lifestyle Modifications
Dietary Changes
Heart-Healthy Diet: A diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can help lower LDL cholesterol levels and reduce inflammation. The Mediterranean diet and the DASH (Dietary Approaches to Stop Hypertension) diet are both associated with cardiovascular benefits.
Reduce Saturated and Trans Fats: Limiting the intake of saturated and trans fats can help manage cholesterol levels. Foods high in these fats include red meat, full-fat dairy products, fried foods, and processed snacks.
Increase Omega-3 Fatty Acids: Consuming sources of omega-3 fatty acids, such as fatty fish (salmon, mackerel, sardines) and flaxseeds, can help reduce inflammation and improve heart health.
Physical Activity
Regular Exercise: Engaging in regular physical activity can help improve cardiovascular health, manage weight, and lower blood pressure. The American Heart Association recommends at least 150 minutes of moderate-intensity aerobic activity per week.
Smoking Cessation
Quit Smoking: Quitting smoking is one of the most effective ways to reduce cardiovascular risk. Smoking cessation programs and support groups can help individuals successfully quit.
Medical Management
Medications
Statins: Statins are commonly prescribed to lower LDL cholesterol levels and reduce the risk of cardiovascular events. They have also been shown to stabilize plaques.
Antihypertensive Medications: Managing high blood pressure with medications can reduce the risk of endothelial injury and plaque progression.
Antiplatelet Agents: Medications such as aspirin may be prescribed to reduce the risk of thrombus formation in individuals with established atherosclerosis.
Management of Comorbid Conditions
Diabetes Management: Controlling blood sugar levels is crucial for individuals with diabetes, as high glucose levels can worsen atherosclerosis.
Weight Management: Achieving and maintaining a healthy weight can help reduce the risk of cardiovascular disease.
Regular Monitoring
Individuals with atherosclerosis should undergo regular monitoring to assess cardiovascular health and identify any changes in plaque formation. This may include routine imaging studies, blood tests, and cardiovascular risk assessments.
Interventional Procedures
In cases of significant arterial blockage due to atherosclerosis, interventional procedures such as angioplasty or bypass surgery may be necessary. These procedures aim to restore blood flow and alleviate symptoms.
The Role of Emerging Therapies
Novel Pharmacological Approaches
Research is ongoing into new therapies that may help target atherosclerosis more effectively. Some promising areas include.
PCSK9 Inhibitors: These medications lower LDL cholesterol levels more aggressively than statins and have shown promise in reducing cardiovascular events.
Anti-inflammatory Therapies: Targeting inflammation directly may help stabilize plaques and reduce cardiovascular risk. Research is being conducted on drugs that inhibit inflammatory pathways involved in atherosclerosis.
Gene Therapy
Emerging research into gene therapy aims to modify genetic factors that contribute to atherosclerosis. While still in the experimental stages, gene therapy may hold potential for future treatment options.
Conclusion
Atherosclerosis is a complex and chronic condition that poses significant risks to cardiovascular health. While it may not completely “go away,” there is substantial evidence that lifestyle modifications, medical management, and emerging therapies can lead to significant improvements in arterial health and potentially reverse some aspects of the disease.
The potential for plaque regression is influenced by various factors, including the duration of the disease, adherence to treatment, and individual genetic predisposition. By adopting heart-healthy lifestyle choices, managing risk factors, and undergoing regular monitoring, individuals can significantly reduce their risk of atherosclerosis and its associated complications.
Healthcare professionals play a crucial role in identifying at-risk individuals, providing appropriate interventions, and promoting awareness of the importance of maintaining cardiovascular health. Through a combination of lifestyle changes, medical therapies, and emerging treatments, it is possible to mitigate the risks associated with atherosclerosis and promote long-term cardiovascular well-being.
Related Topics: