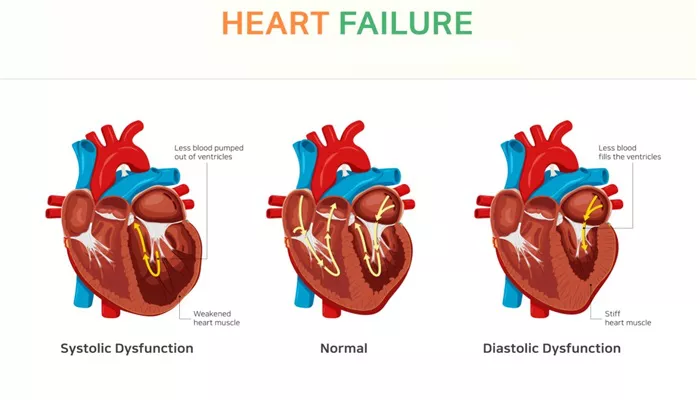
Systolic heart failure, also known as heart failure with reduced ejection fraction (HFrEF), is a serious cardiovascular condition where the heart is unable to pump blood effectively. This condition is one of the most common forms of heart failure, affecting millions of people globally. In systolic heart failure, the heart’s left ventricle, which is responsible for pumping oxygen-rich blood to the body, becomes weakened. As a result, the heart’s ability to contract and circulate blood efficiently is impaired, leading to a reduced ejection fraction (EF). An EF less than 40% is often considered indicative of systolic heart failure.
Heart failure, including systolic heart failure, is a chronic and progressive condition. It can develop over time due to various underlying causes, and without proper management, it can lead to severe complications, including organ damage, disability, and even death. Understanding the causes, symptoms, and treatment methods for systolic heart failure is crucial for both patients and healthcare providers to improve outcomes and enhance the quality of life for those affected.
In this article, we will explore the key aspects of systolic heart failure, including its causes, symptoms, and treatment methods, while also addressing how the condition can be managed to improve patient health and prognosis.
Causes of Systolic Heart Failure
Systolic heart failure can be caused by a variety of factors that either directly damage the heart muscle or lead to conditions that strain the heart over time. The following are the primary causes of systolic heart failure:
1. Coronary Artery Disease (CAD)
Coronary artery disease is the leading cause of systolic heart failure. CAD occurs when the coronary arteries, which supply blood to the heart muscle, become narrowed or blocked by plaque build-up (atherosclerosis). This reduces the blood flow to the heart muscle, leading to ischemia (lack of oxygen). Over time, if left untreated, ischemia can weaken the heart muscle, leading to systolic dysfunction.
2. Myocardial Infarction (Heart Attack)
A heart attack occurs when a blockage in the coronary arteries cuts off the blood supply to a part of the heart muscle. This results in tissue damage and scarring, weakening the heart’s ability to pump effectively. A heart attack is one of the most common causes of systolic heart failure, particularly if the damage is extensive or occurs in a critical area of the heart.
3. Hypertension (High Blood Pressure)
Chronic hypertension places increased strain on the heart. Over time, the heart has to work harder to pump blood against the higher resistance in the blood vessels. This can lead to the thickening of the heart muscle (hypertrophy) and eventually, the weakening of the heart’s pumping ability. If untreated, high blood pressure can contribute to systolic heart failure.
4. Dilated Cardiomyopathy
Dilated cardiomyopathy is a condition where the heart muscle becomes weakened and enlarged. This leads to poor contraction and reduced ejection fraction. The condition can be caused by genetic factors, infections, toxins, alcohol abuse, and certain medications. In some cases, no specific cause is identified (idiopathic dilated cardiomyopathy).
5. Valvular Heart Disease
Valvular heart disease refers to damage or dysfunction of one or more of the heart’s valves. When the heart valves are unable to open or close properly, it causes abnormal blood flow, increasing the workload on the heart. Over time, this can weaken the heart muscle and contribute to systolic heart failure. Common valvular conditions that can cause systolic heart failure include aortic stenosis and mitral regurgitation.
6. Arrhythmias
Certain arrhythmias, particularly sustained atrial fibrillation, can contribute to systolic heart failure. The irregular heart rhythms cause the heart to pump inefficiently, reducing the heart’s ability to circulate blood effectively. Chronic arrhythmias can damage the heart muscle and lead to heart failure over time.
7. Chronic Alcohol Use and Toxins
Chronic alcohol abuse is a known cause of cardiomyopathy and systolic heart failure. Alcohol directly damages heart muscle cells, weakening the heart’s ability to pump blood. Similarly, long-term use of certain medications or exposure to toxic substances can cause heart damage, leading to heart failure.
8. Infections
Viral infections, such as viral myocarditis, can cause inflammation of the heart muscle. If severe or untreated, this inflammation can lead to damage and weakening of the heart muscle, resulting in systolic heart failure.
9. Endocrine Disorders
Conditions such as hyperthyroidism or hypothyroidism, as well as diabetes, can contribute to the development of systolic heart failure. Imbalances in hormones can affect the heart’s ability to function normally, either by increasing the workload on the heart or by directly weakening the heart muscle.
Symptoms of Systolic Heart Failure
The symptoms of systolic heart failure can vary depending on the severity of the condition. Some individuals may experience mild symptoms, while others may suffer from more severe signs. The most common symptoms include:
1. Shortness of Breath (Dyspnea)
Shortness of breath is one of the hallmark symptoms of systolic heart failure. As the heart becomes less efficient at pumping blood, fluid can back up in the lungs, leading to pulmonary congestion. This fluid accumulation makes it harder to breathe, particularly during physical activity or while lying down.
2. Fatigue
Fatigue is a common symptom because the heart is unable to deliver enough oxygen-rich blood to meet the body’s demands. Patients may feel unusually tired and weak, even after minimal exertion.
3. Swelling (Edema)
Swelling in the legs, ankles, feet, and abdomen is common in systolic heart failure. When the heart cannot pump effectively, blood flow becomes congested in the lower extremities, causing fluid retention. This can lead to visible swelling.
4. Reduced Exercise Tolerance
Individuals with systolic heart failure often find it difficult to perform activities that were once easy, such as walking or climbing stairs. The decreased ability of the heart to pump blood efficiently leads to reduced physical stamina.
5. Rapid or Irregular Heartbeat (Palpitations)
As the heart struggles to maintain an adequate blood supply, individuals may experience an increased or irregular heart rate. This can be a result of the heart trying to compensate for its weakened pumping ability.
6. Coughing or Wheezing
Persistent coughing or wheezing, especially when lying down, is another symptom of systolic heart failure. This is caused by fluid accumulation in the lungs, which interferes with normal breathing.
7. Confusion or Impaired Concentration
In some cases, reduced blood flow to the brain can cause confusion, dizziness, or difficulty concentrating. This occurs because the brain is not receiving adequate oxygenated blood.
Treatment Methods for Systolic Heart Failure
Managing systolic heart failure involves a combination of lifestyle changes, medications, and in some cases, surgical interventions. The goal is to relieve symptoms, slow disease progression, and improve the patient’s quality of life.
Treatment strategies include:
1. Medications
Medications are a cornerstone of systolic heart failure treatment. Common classes of drugs used to manage this condition include:
Angiotensin-Converting Enzyme (ACE) Inhibitors: ACE inhibitors help relax blood vessels, reduce blood pressure, and decrease the heart’s workload. They are commonly prescribed to patients with systolic heart failure.
Angiotensin II Receptor Blockers (ARBs): ARBs are similar to ACE inhibitors and are often used when ACE inhibitors are not well tolerated. They also help relax blood vessels and lower blood pressure.
Beta-Blockers: Beta-blockers slow the heart rate and reduce the heart’s workload. They have been shown to improve survival and reduce hospitalizations in patients with systolic heart failure.
Diuretics: Diuretics help reduce fluid retention, which alleviates symptoms of swelling and shortness of breath.
Aldosterone Antagonists: These medications help block the effects of aldosterone, a hormone that can worsen fluid retention and heart failure.
Digitalis (Digoxin): Digitalis can improve the heart’s pumping ability by increasing the strength of each contraction, helping to relieve symptoms of heart failure.
2. Lifestyle Modifications
Lifestyle changes play a critical role in managing systolic heart failure. Key recommendations include:
Dietary Changes: A low-sodium diet is essential to reduce fluid retention. Patients should also monitor their fluid intake to avoid overloading the body with fluids.
Regular Exercise: Though it may seem counterintuitive, regular physical activity, such as walking or swimming, can help strengthen the heart and improve overall health. However, exercise should be tailored to the individual’s tolerance level.
Weight Management: Maintaining a healthy weight can reduce the strain on the heart. Patients should work with their healthcare team to set realistic weight loss goals if necessary.
Quit Smoking: Smoking damages blood vessels and worsens heart failure symptoms. Quitting smoking is one of the most important steps to improve heart health.
Limiting Alcohol: Excessive alcohol intake can worsen heart failure symptoms. Patients with systolic heart failure should limit or avoid alcohol consumption.
3. Surgical and Device Interventions
In some cases, medication and lifestyle changes may not be enough to manage systolic heart failure. Surgical and device-based treatments may be recommended, including:
Coronary Artery Bypass Grafting (CABG): This procedure is used to treat coronary artery disease by bypassing blocked or narrowed arteries, improving blood flow to the heart muscle.
Heart Valve Repair or Replacement: In cases where valvular heart disease contributes to systolic heart failure, surgery to repair or replace the damaged valve may be necessary.
Implantable Cardioverter-Defibrillator (ICD): An ICD is a device implanted in the chest that monitors the heart’s rhythm. It can deliver shocks to restore a normal rhythm in case of life-threatening arrhythmias.
Left Ventricular Assist Device (LVAD): An LVAD is a mechanical pump used to support heart function in patients with severe heart failure. It is typically used as a bridge to heart transplantation or for patients who are not candidates for a transplant.
4. Heart Transplantation
In cases of end-stage systolic heart failure where other treatments are ineffective, heart transplantation may be considered.
This involves replacing the diseased heart with a healthy donor heart. While heart transplantation can significantly improve quality of life, it is not suitable for all patients due to the risks associated with the procedure.
Conclusion
Systolic heart failure is a complex and challenging condition that requires a comprehensive approach to management. By understanding the causes, symptoms, and treatment methods, patients and healthcare providers can work together to slow disease progression and improve quality of life. Advances in medical treatments and surgical interventions continue to enhance the outlook for those living with systolic heart failure. Through early detection, proper management, and lifestyle changes, individuals with systolic heart failure can continue to lead fulfilling and active lives.
Related topics: