Neurogenic orthostatic hypotension (NOH) is a specific type of orthostatic hypotension (OH) that occurs due to dysfunction in the autonomic nervous system (ANS), which controls involuntary bodily functions such as blood pressure regulation, heart rate, digestion, and respiratory rate. NOH is characterized by a significant drop in blood pressure when standing up from a sitting or lying position, leading to symptoms such as dizziness, fainting, and lightheadedness. It is a subtype of orthostatic hypotension that is often associated with neurological conditions.
Unlike other types of orthostatic hypotension, where the drop in blood pressure may be due to factors like dehydration, blood loss, or medication use, neurogenic orthostatic hypotension results from dysfunction in the body’s ability to constrict blood vessels upon standing. This failure to maintain adequate blood pressure can lead to episodes of fainting and a higher risk of falls, which can significantly impair a person’s quality of life.
In this article, we will explore the causes, symptoms, diagnosis, and treatment options for neurogenic orthostatic hypotension, as well as the pathophysiology of this condition.
What Causes Neurogenic Orthostatic Hypotension?
Neurogenic orthostatic hypotension occurs when the autonomic nervous system fails to properly regulate blood pressure in response to changes in posture. This failure can be due to various causes, primarily involving dysfunction of the autonomic nervous system. The main causes of neurogenic orthostatic hypotension include:
1. Parkinson’s Disease and Parkinsonism
Parkinson’s disease, a neurodegenerative disorder, is one of the most common causes of neurogenic orthostatic hypotension. In Parkinson’s disease, the degeneration of dopaminergic neurons in the brain leads to motor symptoms such as tremors, rigidity, and bradykinesia (slowness of movement). Additionally, the loss of autonomic control can lead to a decreased ability to regulate blood pressure, causing orthostatic hypotension. Parkinson’s disease-related NOH is often more difficult to manage due to the progression of the disease.
2. Multiple System Atrophy (MSA)
Multiple system atrophy is another neurodegenerative condition that can cause neurogenic orthostatic hypotension. It is characterized by progressive damage to multiple areas of the brain that control autonomic functions, including blood pressure regulation. In MSA, the inability of the body to constrict blood vessels upon standing leads to a sudden drop in blood pressure, causing symptoms of dizziness and fainting.
3. Pure Autonomic Failure (PAF)
Pure autonomic failure is a rare neurological disorder that primarily affects the autonomic nervous system, impairing its ability to regulate various bodily functions, including blood pressure. In PAF, patients experience orthostatic hypotension due to an impaired ability of the blood vessels to constrict when standing. The condition typically occurs in older adults and is often associated with other autonomic symptoms such as urinary incontinence, constipation, and erectile dysfunction.
4. Diabetic Neuropathy
Long-term uncontrolled diabetes can lead to diabetic neuropathy, a condition where nerve fibers are damaged due to high blood sugar levels. The autonomic nerves that regulate blood pressure can also be affected, leading to neurogenic orthostatic hypotension. Diabetic neuropathy can be particularly challenging to manage, as it may involve both peripheral and autonomic nerves.
5. Amyloidosis
Amyloidosis is a rare condition where abnormal protein deposits (amyloid) accumulate in various organs, including the heart and autonomic nerves. This can interfere with the normal function of the autonomic nervous system and cause neurogenic orthostatic hypotension. Amyloidosis is often associated with other systemic symptoms, such as heart failure, kidney dysfunction, and weight loss.
6. Spinal Cord Injuries
Injury to the spinal cord, particularly at higher levels, can disrupt the communication between the brain and the autonomic nervous system. This disruption can impair the ability to regulate blood pressure, leading to neurogenic orthostatic hypotension. Individuals with spinal cord injuries often experience hypotension upon standing, along with other autonomic symptoms like temperature regulation issues.
7. Neurodegenerative Disorders
In addition to Parkinson’s disease and multiple system atrophy, other neurodegenerative disorders, such as Alzheimer’s disease, may also affect the autonomic nervous system and contribute to the development of neurogenic orthostatic hypotension. These disorders typically involve widespread damage to the brain’s neural pathways, including those that control cardiovascular function.
8. Other Causes
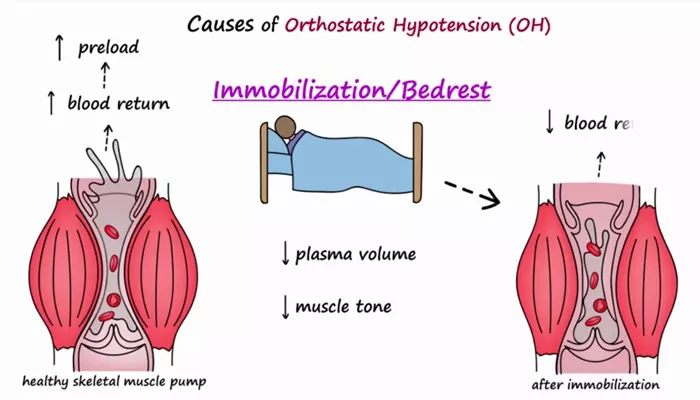
In some cases, neurogenic orthostatic hypotension can result from certain medications (such asthose used to treat high blood pressure, depression, or Parkinson’s disease) or other medical conditions that impair autonomic function. Prolonged bed rest or dehydration can exacerbate symptoms of NOH but are not typically the primary causes of the condition.
Symptoms of Neurogenic Orthostatic Hypotension
The hallmark symptom of neurogenic orthostatic hypotension is a sudden and significant drop in blood pressure when moving from a lying or sitting position to a standing position. This drop in blood pressure can result in a range of symptoms, including:
1. Dizziness and Lightheadedness
One of the first signs of neurogenic orthostatic hypotension is dizziness or lightheadedness upon standing. This occurs when the brain temporarily does not receive enough blood and oxygen due to the drop in blood pressure.
2. Fainting (Syncope)
As the blood pressure drops, the individual may lose consciousness temporarily, leading to fainting. This can be a serious symptom, especially in elderly individuals or those with other medical conditions, as it increases the risk of falls and injuries.
3. Blurred Vision
A sudden drop in blood pressure can cause temporary blurred vision or a sensation of “seeing stars.” This occurs because the eyes are not receiving adequate blood flow during these episodes.
4. Weakness
Patients with neurogenic orthostatic hypotension often experience weakness and fatigue, particularly after standing or engaging in activities that involve posture changes. The muscles may not receive adequate oxygenated blood, leading to feelings of tiredness.
5. Nausea
In some cases, the drop in blood pressure can cause nausea or a general sense of discomfort. This is related to the reduced perfusion of the digestive system and other organs.
6. Headaches
Some individuals with neurogenic orthostatic hypotension may experience headaches, especially if the episodes of hypotension are prolonged. These headaches may be a result of altered blood flow to the brain.
7. Cognitive Dysfunction
In severe cases, individuals with NOH may experience difficulty concentrating, confusion, or problems with memory. This may be due to inadequate blood flow to the brain.
Diagnosis of Neurogenic Orthostatic Hypotension
The diagnosis of neurogenic orthostatic hypotension involves a combination of clinical evaluation, patient history, and diagnostic tests. The main diagnostic criteria for NOH include the following:
1. Clinical Assessment
A healthcare provider will begin with a thorough clinical assessment, including a detailed medical history and review of symptoms. The patient’s symptoms of dizziness or fainting, particularly after standing, will be evaluated.
2. Orthostatic Blood Pressure Measurement
Orthostatic hypotension is diagnosed by measuring blood pressure while the patient is lying down, sitting, and then standing. A significant drop in blood pressure (usually a systolic drop of 20 mmHg or more or a diastolic drop of 10 mmHg or more) upon standing is indicative of orthostatic hypotension.
3. Tilt Table Test
In some cases, a tilt table test may be used to diagnose neurogenic orthostatic hypotension. During this test, the patient is strapped to a table, which is tilted to a standing position while monitoring blood pressure and heart rate. A drop in blood pressure upon standing can confirm the diagnosis.
4. Autonomic Testing
Autonomic function tests can assess the ability of the autonomic nervous system to regulate blood pressure and other bodily functions. These tests can help confirm the diagnosis of neurogenic orthostatic hypotension and identify the underlying cause.
5. Imaging and Laboratory Tests
In some cases, additional imaging studies (such as MRI or CT scans) or laboratory tests may be needed to rule out other underlying conditions, such as brain lesions or metabolic disorders, that could contribute to NOH.
Treatment Methods for Neurogenic Orthostatic Hypotension
The treatment of neurogenic orthostatic hypotension focuses on improving blood pressure regulation, relieving symptoms, and managing the underlying cause. The primary treatment strategies include:
1. Non-Pharmacological Interventions
Lifestyle Modifications: Increasing fluid intake, especially salt-rich fluids, can help increase blood volume and improve blood pressure. Patients are also encouraged to avoid sudden position changes, particularly standing up too quickly.
Compression Garments: Wearing compression stockings or abdominal binders can help reduce blood pooling in the legs and improve blood flow to the brain.
Elevating the Head of the Bed: Raising the head of the bed at night can prevent excessive blood pooling in the lower extremities during sleep, reducing the risk of morning hypotension.
2. Medications
Several medications can help manage neurogenic orthostatic hypotension by improving blood pressure regulation:
Fludrocortisone: A mineralocorticoid that helps increase blood volume and improve blood pressure.
Midodrine: A vasoconstrictor that works by stimulating receptors in blood vessels to increase blood pressure.
Droxidopa: A medication that increases norepinephrine levels, which can help improve vascular tone and blood pressure regulation.
Beta-Blockers: In some cases, beta-blockers may be used to manage symptoms related to heart rate and blood pressure.
3. Treatment of Underlying Conditions
If neurogenic orthostatic hypotension is caused by a neurological condition, such as Parkinson’s disease, multiple system atrophy, or diabetes, managing the underlying disease is crucial. This may involve medications specific to the primary condition, as well as physical therapy to improve balance and mobility.
4. Autonomic Rehabilitation
In some cases, autonomic rehabilitation, which includes exercise programs designed to improve cardiovascular health and autonomic function, may be beneficial. Physical therapy can help improve circulation and blood pressure regulation.
Conclusion
Neurogenic orthostatic hypotension is a complex condition that can significantly impact a patient’s quality of life.
Understanding its causes, symptoms, and treatment options is essential for managing the condition effectively. By addressing both the underlying neurological disorder and the symptoms of low blood pressure, individuals with neurogenic orthostatic hypotension can find relief and improve their functional status.
Related topics: