Chronic Thromboembolic Pulmonary Hypertension (CTEPH) is a rare but serious condition that arises when blood clots (thrombi) that form in the lungs do not resolve properly. These unresolved clots can block the pulmonary arteries, the blood vessels that carry blood from the heart to the lungs, leading to a dangerous increase in pressure within the pulmonary arteries. Over time, this sustained increase in pressure can lead to severe complications, including heart failure.
Unlike acute pulmonary embolism (PE), which is often a one-time event that can be treated with anticoagulation therapy, CTEPH represents a long-term, chronic condition that can develop after an episode of pulmonary embolism, or it may develop without a clear history of PE. It is characterized by persistent obstruction of the pulmonary vasculature, often resulting from the formation of scar tissue in the lungs. This article will delve into the causes, symptoms, diagnosis, and treatment options for CTEPH, and will explore how the condition can be managed to improve patients’ quality of life.
Understanding the Causes of CTEPH
1. Pulmonary Embolism and Incomplete Resolution
The primary cause of CTEPH is a pulmonary embolism that does not fully resolve. When a blood clot or embolism blocks one or more of the pulmonary arteries, it can lead to the death of lung tissue, and the body attempts to repair the damage.
However, in some cases, the blood clot does not break down completely and instead leads to the formation of scar tissue, which obstructs the pulmonary arteries and raises pulmonary artery pressure. This incomplete resolution of an embolism leads to the chronic form of pulmonary hypertension seen in CTEPH.
2. Hypercoagulable States
Some patients are more prone to forming blood clots due to underlying conditions that make their blood “thicker” or more prone to clotting.
These conditions, known as hypercoagulable states, increase the risk of pulmonary embolism and may contribute to the development of CTEPH. Conditions such as antiphospholipid syndrome, Factor V Leiden mutation, and prothrombin gene mutation are known to increase clotting risk.
3. Chronic Inflammation and Vascular Remodeling
Persistent inflammation in the pulmonary arteries following a pulmonary embolism can lead to remodeling of the blood vessels. Over time, this can cause thickening of the vessel walls, further narrowing the arteries, and increasing the pressure in the lungs. This remodeling process is similar to the changes seen in other forms of pulmonary hypertension, but in CTEPH, it occurs specifically in response to the unresolved blood clots.
4. Other Risk Factors
While pulmonary embolism is the leading cause of CTEPH, other risk factors may contribute to the development of the condition. These include:
Surgical procedures: Major surgeries, particularly orthopedic surgeries or those involving prolonged immobility, can increase the risk of deep vein thrombosis (DVT) and subsequent pulmonary embolism.
Cancer: Certain cancers and cancer treatments, especially chemotherapy, can increase the risk of blood clots.
Chronic kidney disease: Renal insufficiency may contribute to a hypercoagulable state and increase the risk of blood clot formation.
Obesity and sedentary lifestyle: Both of these factors can lead to poor circulation and increased risk for thromboembolic events.
Symptoms of CTEPH
The symptoms of CTEPH can vary widely depending on the severity of the pulmonary hypertension and the extent of vascular obstruction. In the early stages, patients may have few or no symptoms. However, as the disease progresses, the following symptoms are commonly observed:
1. Shortness of Breath (Dyspnea)
The hallmark symptom of CTEPH is progressive shortness of breath, especially during physical activity. This occurs because the pulmonary arteries become narrowed and obstructed, reducing the blood flow to the lungs. This results in inadequate oxygenation of the blood and difficulty in maintaining normal breathing, especially during exertion.
2. Fatigue
Patients with CTEPH often experience significant fatigue, which is closely linked to the reduced oxygen supply in the body due to the increased pulmonary pressure. The heart has to work harder to pump blood through the constricted pulmonary vessels, leading to decreased overall energy levels.
3. Chest Pain
Some individuals with CTEPH may experience chest pain, which is typically described as a dull or aching sensation. This pain may occur during physical activity or may be more constant. The chest pain is often caused by the increased pressure in the pulmonary arteries or by right-sided heart strain.
4. Swelling in the Legs and Abdomen (Edema)
As CTEPH progresses and pulmonary pressure increases, the right side of the heart may become strained and less efficient at pumping blood. This can lead to fluid retention in the lower extremities (legs, ankles, and feet) and the abdomen. Swelling can worsen over time and is a sign that the condition is becoming more severe.
5. Syncope (Fainting)
In some cases, patients with CTEPH may experience fainting episodes, particularly during physical exertion. This occurs because the heart’s ability to pump blood effectively is compromised, leading to insufficient blood flow to the brain and other vital organs.
6. Hemoptysis (Coughing up Blood)
In rare cases, patients with CTEPH may experience hemoptysis, or coughing up blood. This is a more severe manifestation of the disease and occurs when the elevated pressure in the pulmonary arteries causes damage to the blood vessels in the lungs.
Diagnosing CTEPH
The diagnosis of CTEPH can be challenging because the symptoms are often similar to other forms of pulmonary hypertension and cardiovascular disease. A thorough clinical evaluation and several diagnostic tests are typically required to confirm the diagnosis of CTEPH. The diagnostic approach includes:
1. Medical History and Physical Examination
A thorough medical history is essential, particularly with respect to any prior history of pulmonary embolism or deep vein thrombosis. Physical examination may reveal signs of right-sided heart failure, such as swelling in the legs, distended neck veins, or abnormal heart sounds.
2. Echocardiogram
An echocardiogram is a non-invasive imaging test that uses sound waves to create images of the heart. It is often the first test used to assess heart function and pulmonary artery pressure. Although echocardiography cannot definitively diagnose CTEPH, it can suggest the presence of pulmonary hypertension and help evaluate the right side of the heart.
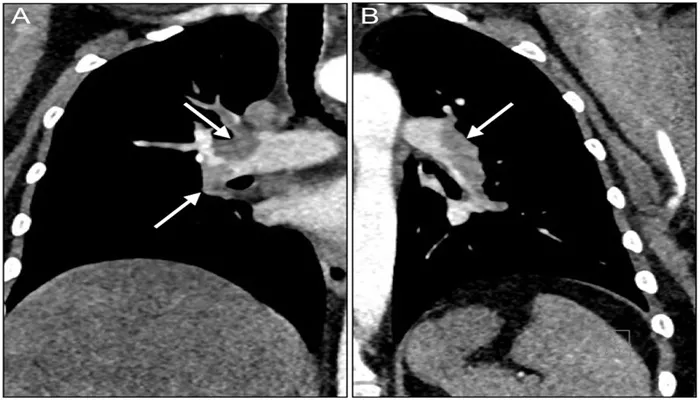
3. Computed Tomography Pulmonary Angiography (CTPA)
CTPA is a key diagnostic tool for identifying blood clots in the lungs. This imaging study can reveal the extent of pulmonary embolism and help assess whether there is evidence of residual clots or scarring that could contribute to CTEPH.
4. Right Heart Catheterization
Right heart catheterization is considered the gold standard for diagnosing pulmonary hypertension, including CTEPH.
During this procedure, a catheter is inserted into the right side of the heart and pulmonary arteries to directly measure the pressure inside the pulmonary arteries. This test helps to confirm the presence of pulmonary hypertension and assess the severity of the disease.
5. Ventilation-Perfusion (V/Q) Scan
A V/Q scan is another imaging test used to evaluate the lungs’ ability to receive oxygen and distribute blood. It can help identify areas of the lung that are poorly perfused (i.e., have inadequate blood flow due to blockages) and may be useful in identifying CTEPH.
Treatment Methods for CTEPH
Treating CTEPH is a complex process that often requires a multi-disciplinary approach. The goal of treatment is to reduce pulmonary artery pressure, improve oxygenation, and enhance the patient’s quality of life. Treatment strategies for CTEPH may include the following:
1. Pulmonary Endarterectomy (PEA)
Pulmonary endarterectomy is a surgical procedure that is considered the most effective treatment for CTEPH in eligible patients. It involves the removal of organized blood clots (endothelial thrombus) from the pulmonary arteries. This procedure is typically performed at specialized centers by skilled surgeons and can significantly improve symptoms and prognosis in appropriate candidates.
2. Balloon Pulmonary Angioplasty (BPA)
In cases where PEA is not feasible, balloon pulmonary angioplasty (BPA) may be an option. BPA is a minimally invasive procedure that uses a balloon catheter to open up narrowed or blocked pulmonary arteries. This procedure is typically performed in patients who are not candidates for surgery or who have persistent symptoms despite surgery.
3. Medications
For patients with CTEPH who are not candidates for surgery, medications may be prescribed to help manage the condition and reduce symptoms. These may include:
Endothelin receptor antagonists (ERAs): These drugs help relax the blood vessels and reduce pulmonary artery pressure.
Phosphodiesterase type 5 inhibitors (PDE-5 inhibitors): These medications work by dilating the blood vessels and improving blood flow in the lungs.
Prostacyclin analogs: These medications are used to dilate the pulmonary arteries and improve blood flow, often administered intravenously or by inhalation.
4. Anticoagulation Therapy
Since CTEPH is closely linked to previous episodes of pulmonary embolism, anticoagulation therapy may be prescribed to prevent further clot formation. Warfarin or direct oral anticoagulants (DOACs) are commonly used in the management of CTEPH to reduce the risk of blood clotting.
5. Oxygen Therapy
For patients with low oxygen levels, supplemental oxygen may be necessary. Oxygen therapy helps to alleviate shortness of breath and improve overall oxygen saturation in the blood.
6. Supportive Care and Lifestyle Modifications
Supportive care, such as physical therapy and pulmonary rehabilitation, can help patients with CTEPH improve exercise tolerance and quality of life. Additionally, lifestyle modifications such as weight management and smoking cessation are important in managing the condition and reducing the risk of complications.
Conclusion
Chronic Thromboembolic Pulmonary Hypertension (CTEPH) is a serious and potentially life-threatening condition that can arise following pulmonary embolism. While it is a rare disease, it is important to recognize its symptoms, understand its causes, and provide appropriate treatment to improve the patient’s prognosis and quality of life. Early diagnosis and a tailored approach to treatment, including surgery and medications, can help manage the disease effectively. With ongoing advances in medical treatments and surgical techniques, there is hope for patients with CTEPH to lead fulfilling lives.
Related topics: