Myocardial edema is a term used to describe the swelling or fluid accumulation within the heart muscle (myocardium). This condition, while often linked to various heart diseases and acute events such as myocardial infarction (heart attack), can also be seen in other cardiovascular conditions. Myocardial edema can lead to a series of complications that can further compromise heart function and overall health. In this comprehensive guide, we will explore the definition, causes, symptoms, diagnostic techniques, treatment options, and potential outcomes of myocardial edema. By understanding this condition in greater detail, healthcare professionals and patients can be better equipped to handle its implications.
Understanding Myocardial Edema
At its core, myocardial edema is a result of an imbalance between the processes of fluid movement and regulation within the heart muscle. Normally, the heart muscle remains in a delicate state of fluid homeostasis. However, when this balance is disturbed, it leads to excess fluid buildup in the tissue, causing swelling and inflammation. This swelling can reduce the heart’s efficiency in pumping blood, leading to further health complications.
The heart muscle, like any other tissue in the body, requires adequate blood flow and oxygenation to function optimally. When these needs are not met, it can trigger inflammatory processes that may result in fluid accumulation. Myocardial edema may present itself as a subtle condition, but its implications can be far-reaching if left untreated.
Causes of Myocardial Edema
There are several causes of myocardial edema, which often occur as part of larger cardiovascular or systemic issues. Some of the most common causes include:
1. Acute Myocardial Infarction (Heart Attack)
Myocardial edema is most commonly seen after a heart attack. When a part of the heart’s blood supply is blocked, the affected tissue becomes deprived of oxygen and nutrients. This ischemic injury leads to inflammation and edema as the body responds to the damage. The swelling in the heart muscle can impede its ability to pump effectively, contributing to further complications such as heart failure or arrhythmias.
2. Myocarditis
Myocarditis, an inflammation of the heart muscle, is another common cause of myocardial edema. In this condition, the heart muscle becomes inflamed due to an infection, autoimmune disorder, or other factors. The inflammation leads to fluid buildup within the heart tissue. The severity of myocardial edema in myocarditis depends on the extent of inflammation and the underlying cause.
3. Heart Failure
Chronic heart failure, especially when associated with left ventricular dysfunction, can also result in myocardial edema. In heart failure, the heart’s ability to pump blood is compromised, leading to fluid retention throughout the body. This retained fluid can accumulate in the heart muscle, exacerbating the heart’s inefficiency.
4. Cardiomyopathy
Cardiomyopathy refers to a group of diseases that affect the heart muscle, leading to changes in its structure and function. In some cases, cardiomyopathy causes swelling and fluid buildup in the myocardium. This may occur due to various factors, including genetic mutations, chronic high blood pressure, or alcohol use.
5. Post-Cardiac Surgery or Trauma
Patients who undergo heart surgery or experience trauma to the chest may develop myocardial edema as part of the healing process. The trauma or surgical incision can lead to inflammation in the heart muscle, causing localized swelling and fluid accumulation. This is typically a temporary condition, but it requires careful monitoring to ensure that it does not cause further complications.
6. Systemic Conditions
Certain systemic conditions, such as hypertension, diabetes, or kidney disease, can contribute to myocardial edema. High blood pressure, for instance, puts added strain on the heart, potentially leading to swelling and edema in the myocardial tissue. Additionally, diseases affecting fluid regulation, such as kidney failure, can increase the likelihood of fluid retention within the heart.
Symptoms of Myocardial Edema
The symptoms of myocardial edema can vary depending on the underlying cause, the severity of the swelling, and the area of the heart affected. Common symptoms include:
Chest pain: Swelling in the myocardium may cause discomfort or pain in the chest, especially if it results from a heart attack or myocarditis.
Fatigue: As the heart struggles to pump effectively, patients may experience fatigue or shortness of breath.
Shortness of breath: This can be especially noticeable when performing physical activities or when lying flat, as fluid may accumulate in the lungs in severe cases.
Swelling in the legs and ankles: Fluid buildup in the body, often due to heart failure, can cause peripheral edema, particularly in the lower extremities.
Irregular heartbeats (arrhythmias): Myocardial edema can disrupt the electrical pathways of the heart, leading to arrhythmias such as palpitations or rapid heart rate.
Dizziness or fainting: Decreased cardiac output due to myocardial edema can result in dizziness or syncope (fainting), especially when standing up quickly.
Diagnosing Myocardial Edema
The diagnosis of myocardial edema typically involves a combination of clinical evaluation, imaging studies, and laboratory tests. Some of the most common diagnostic methods include:
1. Echocardiography
Echocardiography uses sound waves to create an image of the heart, helping doctors visualize its size, shape, and function.
In cases of myocardial edema, echocardiograms can reveal areas of swelling or changes in the heart’s function. The test can also identify fluid buildup within the heart chambers or surrounding tissue.
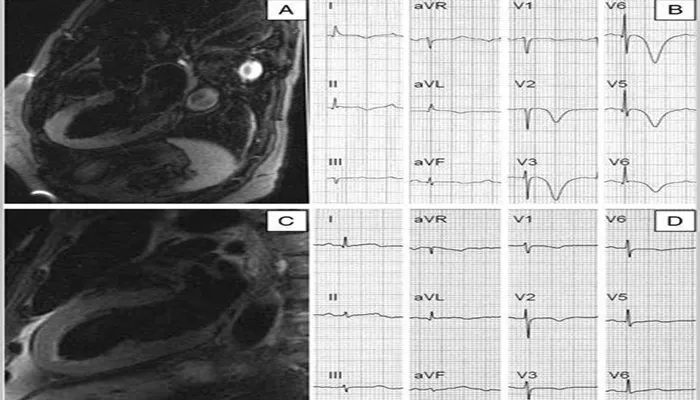
2. Magnetic Resonance Imaging (MRI)
Cardiac MRI is a highly sensitive imaging technique that can assess the extent of myocardial edema. MRI scans provide detailed images of the heart muscle, allowing doctors to detect subtle changes in tissue composition and identify areas of inflammation or swelling.
3. Blood Tests
Blood tests are useful in detecting markers of inflammation and assessing the overall health of the heart. Elevated levels of certain biomarkers, such as troponin, can indicate myocardial injury or inflammation, suggesting the presence of myocardial edema.
4. Computed Tomography (CT) Scan
CT scans are sometimes used to assess the heart and its surrounding structures. While not as commonly used as echocardiography or MRI, CT imaging can help identify areas of fluid buildup or structural changes associated with myocardial edema.
5. Biopsy
In rare cases, a heart biopsy may be performed to collect tissue samples for analysis. This is typically done in situations where the cause of myocardial edema is unclear or when autoimmune or infectious myocarditis is suspected.
Treatment of Myocardial Edema
The treatment of myocardial edema depends largely on the underlying cause and the severity of the condition. Some common treatment strategies include:
1. Medications
Diuretics: To reduce fluid buildup in the body, diuretics may be prescribed to promote urination and decrease the strain on the heart.
Anti-inflammatory drugs: If myocardial edema is caused by inflammation, medications such as corticosteroids or nonsteroidal anti-inflammatory drugs (NSAIDs) may be used to reduce swelling.
ACE inhibitors and beta-blockers: These medications are often used to treat heart failure or myocardial infarction by improving heart function and reducing blood pressure.
Antibiotics or antivirals: If myocardial edema is caused by an infection, appropriate medications to target the infection will be necessary.
2. Lifestyle Changes
Patients with myocardial edema may be advised to make certain lifestyle modifications to help reduce the burden on the heart. These changes may include:
Limiting salt intake to reduce fluid retention.
Maintaining a healthy weight to ease strain on the heart.
Engaging in moderate physical activity, if recommended by a doctor, to improve heart function.
Quitting smoking and reducing alcohol consumption to support overall cardiovascular health.
3. Surgery or Interventional Procedures
In severe cases, surgical or interventional procedures may be necessary. For example, patients with a significant blockage in the coronary arteries may require coronary artery bypass surgery or angioplasty to restore proper blood flow to the heart muscle. Similarly, patients with severe myocarditis may need procedures to address heart failure or arrhythmias.
Conclusion
Myocardial edema is a serious condition that can lead to a range of cardiovascular complications if left untreated. Understanding its causes, symptoms, and treatment options is vital for both healthcare providers and patients. Early detection and management can significantly improve outcomes, helping individuals maintain better heart health and quality of life. By focusing on the underlying cause and implementing appropriate interventions, myocardial edema can be effectively managed, reducing the risk of long-term heart damage.
Related topics: