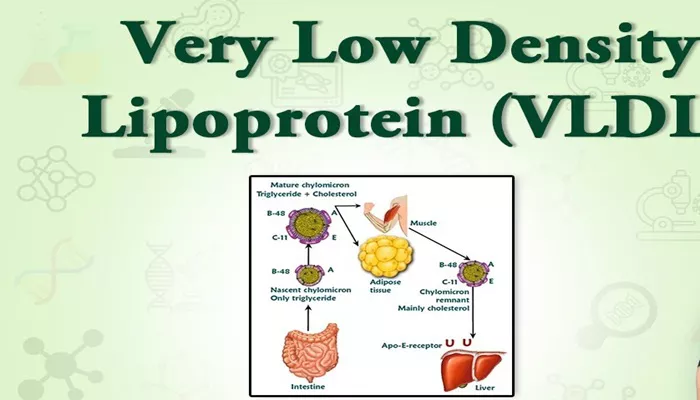
Very-low-density lipoprotein (VLDL) is one of the five major lipoproteins that play a crucial role in the transportation of lipids (fats) throughout the body. It is primarily responsible for carrying triglycerides, a type of fat, from the liver to peripheral tissues. Elevated levels of VLDL are associated with an increased risk of cardiovascular diseases, including atherosclerosis and coronary artery disease (CAD). Understanding VLDL, its function, health implications, and ways to manage its levels is essential for maintaining heart health.
In this comprehensive guide, we will delve into the functions, composition, health risks, diagnostic methods, and management strategies related to VLDL.
What Is Very-Low-Density Lipoprotein (VLDL)?
VLDL is a type of lipoprotein produced by the liver to transport triglycerides and other lipids through the bloodstream. It belongs to the lipoprotein family, which includes:
- High-density lipoprotein (HDL) – “Good” cholesterol
- Low-density lipoprotein (LDL) – “Bad” cholesterol
- Intermediate-density lipoprotein (IDL)
- Chylomicrons
VLDL is considered a “bad” lipoprotein because, like LDL, it contributes to plaque buildup in the arteries, which can lead to cardiovascular disease.
The Composition and Function of VLDL
Lipid Content
VLDL is primarily composed of:
Triglycerides (55-65%) – The predominant lipid in VLDL, which serves as an energy source.
Cholesterol (10-15%) – A structural component of cells and precursor to hormones.
Phospholipids (15-20%) – Essential for cell membrane integrity.
Apolipoproteins (10%) – Proteins that help VLDL function properly.
Function in Lipid Transport
VLDL plays a crucial role in transporting triglycerides from the liver to adipose and muscle tissues for energy storage and utilization. Once VLDL releases triglycerides, it transforms into intermediate-density lipoprotein (IDL), which can further become LDL.
How VLDL Contributes to Atherosclerosis
VLDL, like LDL, is considered atherogenic, meaning it promotes plaque formation in the arteries. This occurs through the following process:
Triglyceride deposition – Excess VLDL leads to increased triglycerides in the blood.
Transformation into LDL – After delivering triglycerides, VLDL becomes LDL, which is more likely to deposit cholesterol in artery walls.
Inflammation and Plaque Formation – The presence of VLDL and LDL triggers an inflammatory response, leading to plaque buildup.
Risk Factors for Elevated VLDL
Several factors contribute to high VLDL levels, including:
Poor diet – Excess intake of refined carbohydrates and saturated fats.
Obesity – Increased fat storage raises triglyceride production.
Sedentary lifestyle – Lack of physical activity impairs lipid metabolism.
Diabetes and insulin resistance – Disrupted lipid balance can elevate VLDL levels.
Genetic predisposition – Some individuals inherit a tendency for high VLDL levels.
How VLDL Levels Are Measured
VLDL Estimation in Blood Tests
VLDL levels are typically not measured directly. Instead, they are estimated using the following formula:
VLDL = Triglycerides/5 (in mg/dL)
This calculation is based on the assumption that VLDL carries approximately one-fifth of circulating triglycerides. However, for more precise measurements, advanced lipid testing methods such as ultracentrifugation or nuclear magnetic resonance (NMR) spectroscopy may be used.
Normal and High VLDL Levels
- Normal range: 2-30 mg/dL
- Borderline high: 30-40 mg/dL
- High: >40 mg/dL
High VLDL levels indicate an increased risk for heart disease and metabolic disorders.
Strategies to Lower VLDL Levels
1. Dietary Modifications
Reduce sugar and refined carbohydrate intake – High sugar consumption increases triglyceride production.
Increase healthy fats – Replace saturated fats with omega-3 fatty acids (found in fish, flaxseeds, and walnuts).
Consume fiber-rich foods – Whole grains, vegetables, and legumes help lower triglycerides.
2. Exercise and Physical Activity
Engaging in aerobic exercise (e.g., walking, jogging, cycling) helps burn triglycerides and lowers VLDL levels.
Strength training supports overall metabolism and lipid balance.
3. Weight Management
Losing excess weight reduces triglyceride production, lowering VLDL and overall cardiovascular risk.
4. Medication Therapy
For individuals with persistently high VLDL levels, medications may be necessary. These include:
Statins – Lower cholesterol and reduce cardiovascular risk.
Fibrates – Target triglycerides and VLDL reduction.
Niacin (Vitamin B3) – Helps lower triglyceride levels.
Omega-3 fatty acids (Prescription forms like Lovaza) – Improve lipid profiles.
5. Lifestyle Changes
Quit smoking – Smoking worsens lipid metabolism and contributes to arterial plaque.
Limit alcohol consumption – Alcohol can increase triglyceride levels.
Manage stress – Chronic stress affects metabolic health, raising VLDL levels.
Conclusion
Very-low-density lipoprotein (VLDL) is a crucial player in lipid metabolism but can contribute to cardiovascular disease when present in high amounts. Managing VLDL levels through a balanced diet, regular exercise, and, when necessary, medication can significantly reduce the risk of heart disease. Regular monitoring of lipid levels and proactive lifestyle changes are essential for maintaining optimal heart health.
Related topics: